Steady fixation is considered roughly equivalent to 20/40, unsteady fixation is equivalent to 20/100, and inability to fixate is equivalent to 20/400. A light source should be used 1-3 feet away the ability to track and fixate on light determines adequate visual acuity. Visual acuity in the neonate, infant, and toddlers is performed by assessing pupillary reaction to light. Visual acuity should never be excluded and the only time that it should be postponed is when a patient presents with a chemical exposure to the eye requiring immediate irrigation. Inadvertent peeking around a parent's hand or wand occluder can lead to a false determination of vision in the traumatized eye. An adhesive eye patch should be used for the assessment of vision in children. Visual acuity is the vital sign of the eye, and is absolutely essential in the evaluation of eye trauma. Remember to perform the more uncomfortable portions of the examination last. 9 However, certain areas of a thorough eye examination are age specific, other areas are independent of age, and most depend on patient cooperation. After collecting a comprehensive history, the physical examination of the eye should include these elements: visual acuity, pupillary reactions, external examination, ocular motility, visual field testing, slit-lamp examination, fluorescein staining, intraocular pressure, and funduscopic examination. Topical anesthesia may give the patient comfort during the eye examination. Most patients older than age 3 can be successfully examined using interactive distracting techniques and parental assistance rarely, a papoose board or sedation may be required to complete an adequate examination. 7,8Įxamination of the Injured Eye in the Pediatric PatientĮxamining the injured eye of a pediatric patient may pose a significant challenge. 6 It is important to note, however, that eye injuries also may be associated with major trauma, particularly in patients with facial fractures, facial contusions, or basilar skull fractures patients require a comprehensive evaluation to exclude concomitant injuries. Many eye injuries can be prevented by appropriate supervision of children's activities and the appropriate use of protective eye wear during sports.Įye injuries often are isolated injuries and may be managed as outpatients Approximately 2-3% of patients require inpatient hospital admission. 4,5 Ocular trauma is one of the most significant causes of visual loss in pediatric patients. 3 The most common injuries include corneal abrasion, blunt trauma, and corneal foreign body. 
1,2 The majority of injuries occur in the home, followed by public places, such as schools or athletic facilities. It is estimated that 2.4 million eye injuries occur annually in the United States, accounting for 0.2% of ED visits approximately one-third of eye injuries occur in pediatrics. The authors present a complete review of the evaluation and management of the patient with a potential eye injury.Įye trauma is a common chief complaint among ED patients. Certain eye injuries warrant ophthalmologic consultation, including hyphema, penetrating globe injury, suspected or known open globe injury, retrobulbar hematoma, or any eye injury resulting in significant visual loss. 
Certain "tricks of the trade" are presented here to aid the clinician in obtaining this critical information.įollowing complete evaluation, many patients with eye injuries can be managed as outpatients with appropriate medical management and ophthalmologic follow-up. 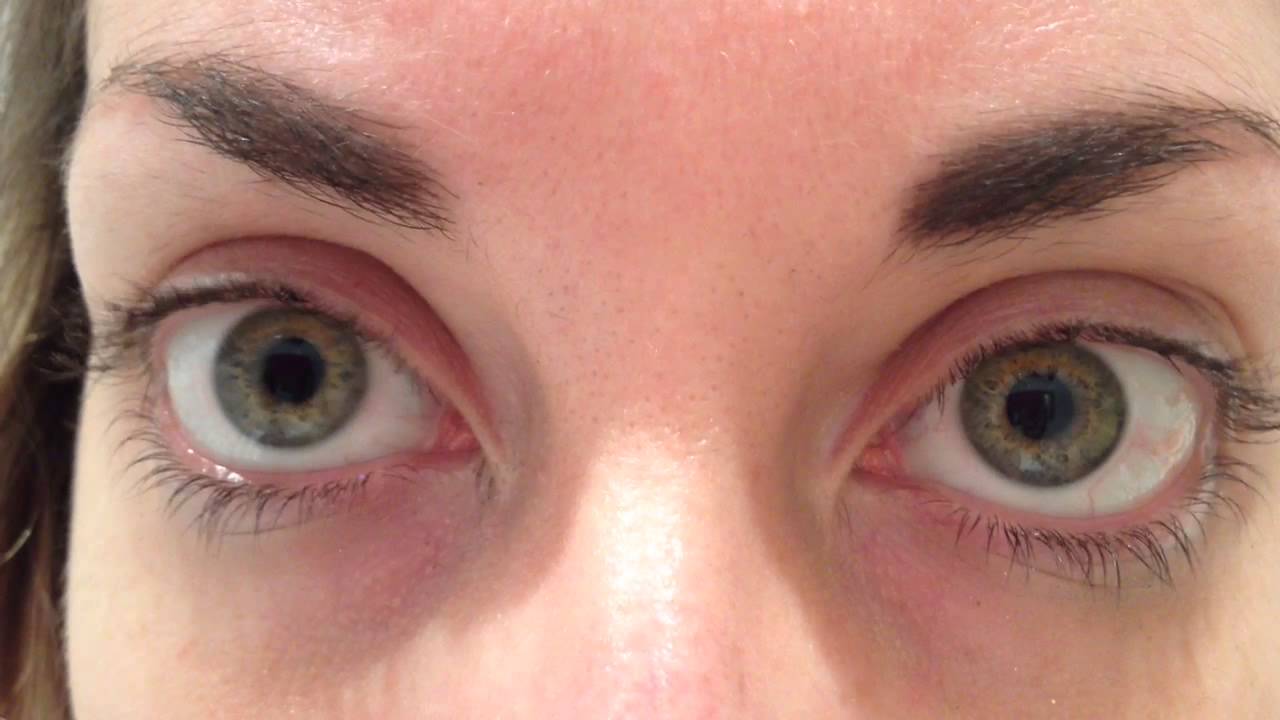
Specific attention to the physical examination is mandatory in the evaluation of pediatric eye trauma, and although challenging should include visual acuity, pupillary reactions, external examination, ocular motility, visual field testing, slit-lamp examination, fluorescein staining, intraocular pressure, and funduscopic examination. Although many eye injuries can be prevented by appropriate supervision of children's activities and the appropriate use of protective eye wear, eye injuries remain an important cause of visual loss. Peer reviewer: Melanie Kazlas, MD, Acting Director, Pediatric Ophthalmology and Strabismus, Massachusetts Eye and Ear Infirmary, Harvard Medical School.Įye trauma is a common chief complaint among emergency department (ED) pediatric patients. Vincent Mercy Medical Center, Toledo, OH. Vincent Mercy Medical Center, Toledo, OH and Jeffrey Salisbury, MD, St. Marco, MD, FACEP, Clinical Professor, Surgery, Medical University of Ohio, Attending Physician, St. Keeping an "Eye" on the Patient: Pediatric Eye TraumaĪuthors: Catherine A.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
